Understanding Corneal Transplant
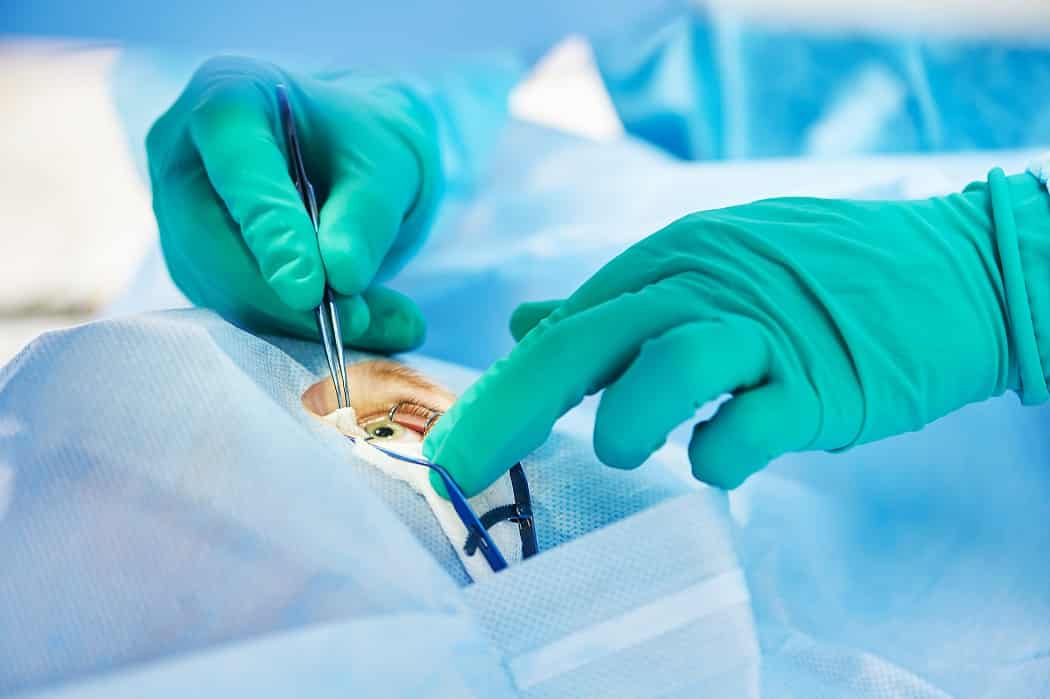
A corneal transplant, also known as keratoplasty, is a surgical procedure designed to replace a damaged or diseased cornea with a healthy donor cornea. The cornea is the transparent, dome-shaped layer at the front of the eye that focuses light onto the retina, playing a critical role in clear vision. When the cornea becomes scarred, diseased, or misshapen due to conditions like keratoconus, infections, injuries, or corneal dystrophies, vision can be severely impaired. Corneal transplant restores vision by replacing the affected corneal tissue, allowing light to pass properly through the eye. The procedure can improve not only vision but also the overall quality of life for patients who struggle with impaired sight. The decision to undergo a corneal transplant is made after a thorough evaluation by an ophthalmologist, who assesses the severity of corneal damage and the patient’s overall eye health. With modern surgical techniques, corneal transplants have become increasingly successful, offering long-term benefits for patients of all ages.
Types of Corneal Transplants
Corneal transplants are classified based on the layers of the cornea being replaced. One common type is Penetrating Keratoplasty, which involves replacing the full thickness of the cornea. Lamellar Keratoplasty is a partial-thickness transplant that targets only the damaged layer while leaving healthy tissue intact. Endothelial Keratoplasty focuses on replacing only the innermost corneal layer, making it less invasive and providing faster recovery. Each type has distinct advantages depending on the patient’s condition, age, and desired visual outcomes. Full-thickness transplants are ideal for severe scarring or thinning, while partial transplants reduce risks such as graft rejection. Surgeons choose the type based on the exact location and extent of corneal damage. Understanding these options helps patients make informed decisions about their eye health.
The Corneal Transplant Procedure
Before undergoing a corneal transplant, patients undergo comprehensive eye exams and medical evaluations to ensure they are suitable candidates. The procedure can be performed under local or general anesthesia, depending on the patient’s comfort level and the complexity of the surgery. During the surgery, the surgeon carefully removes the damaged cornea and replaces it with donor tissue, securing it in place with tiny sutures or specialized techniques. The procedure generally takes one to two hours, but recovery time varies depending on the type of transplant and individual healing. Following surgery, patients are monitored closely for any signs of complications or infection. Proper post-operative care, including the use of prescribed eye drops and medications, plays a crucial role in successful outcomes. Patients are encouraged to follow their surgeon’s instructions carefully to ensure the graft integrates properly and vision improves over time.
Risks and Potential Complications
While corneal transplants are generally safe, like all surgeries, they carry certain risks. Graft rejection is one of the most common complications, where the body’s immune system identifies the new cornea as foreign and attacks it. Symptoms of rejection may include redness, sensitivity to light, vision changes, or discomfort. Infection is another concern, which can be minimized through sterile surgical procedures and diligent post-operative care. Other potential issues include glaucoma, irregular astigmatism, or suture-related problems. The risk of complications can be reduced by selecting a skilled surgeon, following all post-surgery guidelines, and attending regular check-ups. Prompt detection and management of any problems significantly improve the likelihood of a successful outcome. Understanding these risks empowers patients to take an active role in their recovery.
Recovery and Aftercare
Recovery after a corneal transplant requires patience and careful attention to the eye. Most patients notice improvements in vision within weeks, but complete visual recovery can take several months to a year, depending on the type of transplant. Eye drops, including antibiotics and anti-rejection medications, are prescribed to prevent infection and support graft acceptance. Certain activities, such as heavy lifting, swimming, or rubbing the eyes, should be avoided during the healing period. Regular follow-up appointments with the ophthalmologist are critical to monitor healing, detect any early signs of complications, and adjust medications as needed. Maintaining good eye hygiene and protecting the eyes from injury or bright sunlight also contribute to a successful recovery. Patients who adhere to these guidelines are more likely to enjoy long-lasting improvements in vision and eye health.
Advancements in Corneal Transplant
Corneal transplant procedures have advanced significantly over the past few decades. Modern techniques, such as femtosecond laser-assisted transplants, allow surgeons to create precise corneal cuts, improving graft fit and reducing healing time. Artificial corneas, known as keratoprostheses, are now available for patients who cannot receive traditional donor tissue. Researchers are exploring regenerative therapies and stem cell applications to restore corneal tissue without the need for full transplants. These innovations are making the procedure safer, more efficient, and accessible to a broader range of patients. Surgical techniques continue to evolve, offering higher success rates and faster recovery. Staying informed about these advancements can help patients and their families feel confident in their treatment options.
Choosing the Right Eye Specialist
Selecting a qualified corneal surgeon is essential for a successful transplant. Patients should consider factors such as the surgeon’s experience, certifications, and track record with corneal procedures. Asking questions about the surgery, recovery expectations, and potential risks ensures that patients make informed decisions. Seeking a second opinion may provide additional reassurance and help clarify treatment options. Communication between the patient and surgeon is critical to managing expectations and achieving optimal outcomes. Hospitals and clinics with specialized cornea departments often offer the most advanced care. Patients are encouraged to research thoroughly and choose a provider they trust and feel comfortable with.
Living with a Corneal Transplant
Adapting to life after a corneal transplant involves adjusting to changes in vision and maintaining long-term eye health. Vision may fluctuate during the initial months, and glasses or contact lenses might be necessary to fine-tune clarity. Patients should avoid activities that could injure the eye, and wearing protective eyewear is recommended for sports or high-risk environments. Regular check-ups help monitor for late-onset complications, including graft rejection that can occur years after surgery. Eye care routines, such as proper hygiene and consistent use of prescribed medications, are essential for long-term success. Support groups and patient resources can offer emotional support and practical advice. With proper care and monitoring, many patients enjoy a significant improvement in quality of life and visual function.
Frequently Asked Questions (FAQ)
How long does a corneal transplant last?
Corneal transplants can last for many years, often 10 to 20 years or more. Longevity depends on factors like patient health, type of transplant, and adherence to aftercare instructions.
What is the success rate of corneal transplants?
Success rates vary depending on the procedure type and underlying condition but are generally high, with many patients achieving substantial vision improvement.
Can both eyes undergo a transplant simultaneously?
It is uncommon for both eyes to be transplanted at the same time. Usually, one eye is treated first to minimize risk and monitor healing.
Is corneal transplant painful?
The procedure itself is usually painless due to anesthesia. Post-operative discomfort is generally mild and managed with prescribed medications.
How soon can normal activities resume after surgery?
Patients are advised to avoid strenuous activities for several weeks. Light daily activities can often resume within a few days to weeks, depending on the type of transplant.
Can the cornea reject years after transplant?
Yes, graft rejection can occur even years later. Prompt attention to symptoms like redness, light sensitivity, or blurred vision is crucial for treatment.
Takeaway
A corneal transplant offers hope for patients with severe corneal damage, restoring vision and improving quality of life. With advances in surgical techniques and post-operative care, the procedure has become safer and more effective than ever. Understanding the types of transplants, potential risks, and recovery requirements empowers patients to make informed decisions. Choosing the right surgeon, adhering to aftercare instructions, and maintaining long-term eye health are essential for success. Modern innovations, including laser-assisted techniques and artificial corneas, continue to expand the possibilities for treatment. For anyone experiencing vision impairment due to corneal disease, a corneal transplant provides a pathway to clearer vision and renewed independence. With proper care, patience, and professional guidance, patients can enjoy the long-lasting benefits of this life-changing procedure.