Pressure sores are a serious concern for bedridden patients, often leading to discomfort, infections, and complications if left untreated. Proper pressure sore treatment is essential to protect the skin, prevent further deterioration, and improve overall well-being. Patients and caregivers must understand effective care strategies and seek professional support when necessary. Kalingap Wound Care Clinic stands out as a trusted provider of specialized pressure sore management, offering comprehensive care tailored to each patient’s needs.
What Are Pressure Sores?
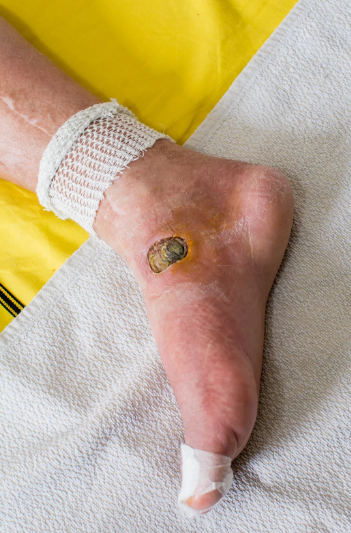
Pressure sores, also known as bedsores or decubitus ulcers, occur when prolonged pressure restricts blood flow to the skin and underlying tissues. They commonly develop over bony areas such as the heels, tailbone, elbows, and hips. Pressure sores are classified into stages from Stage 1, showing redness and irritation, to Stage 4, characterized by deep tissue damage and potential infection. Recognizing these stages early is vital for effective pressure sore treatment and prevention of complications.
Causes of Pressure Sores in Bedridden Patients
Bedridden patients are particularly vulnerable due to limited mobility. Prolonged pressure on specific areas compresses blood vessels, causing tissue damage over time. Friction and shear forces from movement in bed can worsen skin breakdown. Additional factors such as excessive moisture, poor nutrition, and underlying health conditions like diabetes or circulatory disorders increase susceptibility. Addressing these causes promptly is essential for successful pressure sore treatment.
Signs and Symptoms to Watch For
Early detection is critical for effective pressure sore treatment. Common signs include redness, swelling, or skin discoloration that does not fade when pressure is relieved. Patients may experience tenderness or pain in affected areas. In more advanced stages, open wounds, blisters, and signs of infection such as pus or foul odor may appear. Observing these symptoms allows caregivers and medical professionals to implement treatment strategies before complications develop.
Preventive Measures for Bedridden Patients
Preventing pressure sores is a key aspect of patient care. Regular repositioning every two hours helps relieve pressure on vulnerable areas. Pressure-relieving mattresses, cushions, and pads provide additional protection. Maintaining proper hygiene and keeping the skin clean and dry reduce infection risks. Adequate nutrition and hydration also support skin integrity and overall health. Following these preventive measures complements ongoing pressure sore treatment for patients at risk.
Pressure Sore Treatment Options
Non-Surgical Treatments
Non-surgical pressure sore treatment focuses on wound care, infection prevention, and pain management. This includes cleaning the wound with appropriate solutions, applying medicated dressings, and using topical antibiotics when necessary. Pain relief and anti-inflammatory measures ensure patient comfort while promoting healing. Regular monitoring of wound progress is essential to adjust treatment plans effectively.
Surgical Treatments
Severe pressure sores may require surgical intervention. Procedures such as debridement remove necrotic tissue to prevent infection and promote recovery. In some cases, skin grafts or flap surgeries may be necessary to restore damaged areas. Surgical pressure sore treatment is typically combined with professional wound care to ensure optimal healing and prevent recurrence.
Role of Professional Care
Professional care is essential for effective pressure sore treatment, particularly for patients with complex or advanced wounds. Clinics like Kalingap Wound Care Clinic provide specialized care, including personalized treatment plans, continuous monitoring, and infection management. Their expert staff ensures patients receive the highest standard of wound care, improving recovery outcomes and quality of life.
Home Care Tips for Pressure Sore Management
Caregivers play a vital role in supporting pressure sore treatment at home. Gentle repositioning techniques reduce friction and pressure. Keeping the skin clean and dry, applying protective dressings, and using barrier creams help prevent further damage. Monitoring wounds closely and reporting changes to a professional ensures timely intervention and better healing outcomes.
Complications of Untreated Pressure Sores
Ignoring pressure sores can lead to severe complications. Infections may progress to sepsis, posing life-threatening risks. Deep tissue damage can affect muscles and bones, causing long-term mobility issues. Untreated pressure sores often require hospitalization and extensive medical care, highlighting the importance of early pressure sore treatment and ongoing management.
Choosing the Right Clinic for Pressure Sore Treatment
Selecting a qualified clinic is crucial for effective pressure sore treatment. Key factors include experienced medical staff, modern equipment, and customized care plans. Kalingap Wound Care Clinic excels in all these areas, offering reliable treatment, expert guidance, and comprehensive monitoring. Patients and caregivers can trust the clinic to provide attentive care that prioritizes healing, comfort, and overall health.
Takeaway
Pressure sores pose a serious threat to bedridden patients, making prompt and proper pressure sore treatment essential. Early detection, preventive measures, and professional care significantly improve outcomes and quality of life. Trusting experts like Kalingap Wound Care Clinic ensures patients receive personalized, high-quality care that addresses both healing and comfort. Prompt intervention and consistent management are the keys to preventing complications and supporting full recovery.
Frequently Asked Questions (FAQ)
How long does it take for a pressure sore to heal?
Healing time depends on the stage and severity of the sore. Early-stage sores may heal in a few days with proper treatment, while advanced sores may require weeks or months, especially under professional care from Kalingap Wound Care Clinic.
Can pressure sores be completely prevented?
Yes, with regular repositioning, proper skin care, and supportive equipment, many pressure sores can be prevented. Prevention combined with early pressure sore treatment significantly reduces risks.
Are pressure sores covered by insurance?
Coverage depends on the patient’s insurance plan. Many health plans include wound care services, especially when prescribed by a medical professional for chronic or severe cases.
How often should bedridden patients be repositioned?
Caregivers should reposition patients at least every two hours to relieve pressure and support skin health. Combining this with professional guidance enhances pressure sore treatment effectiveness.