Understanding Wound Care Assessment and Its Clinical Importance
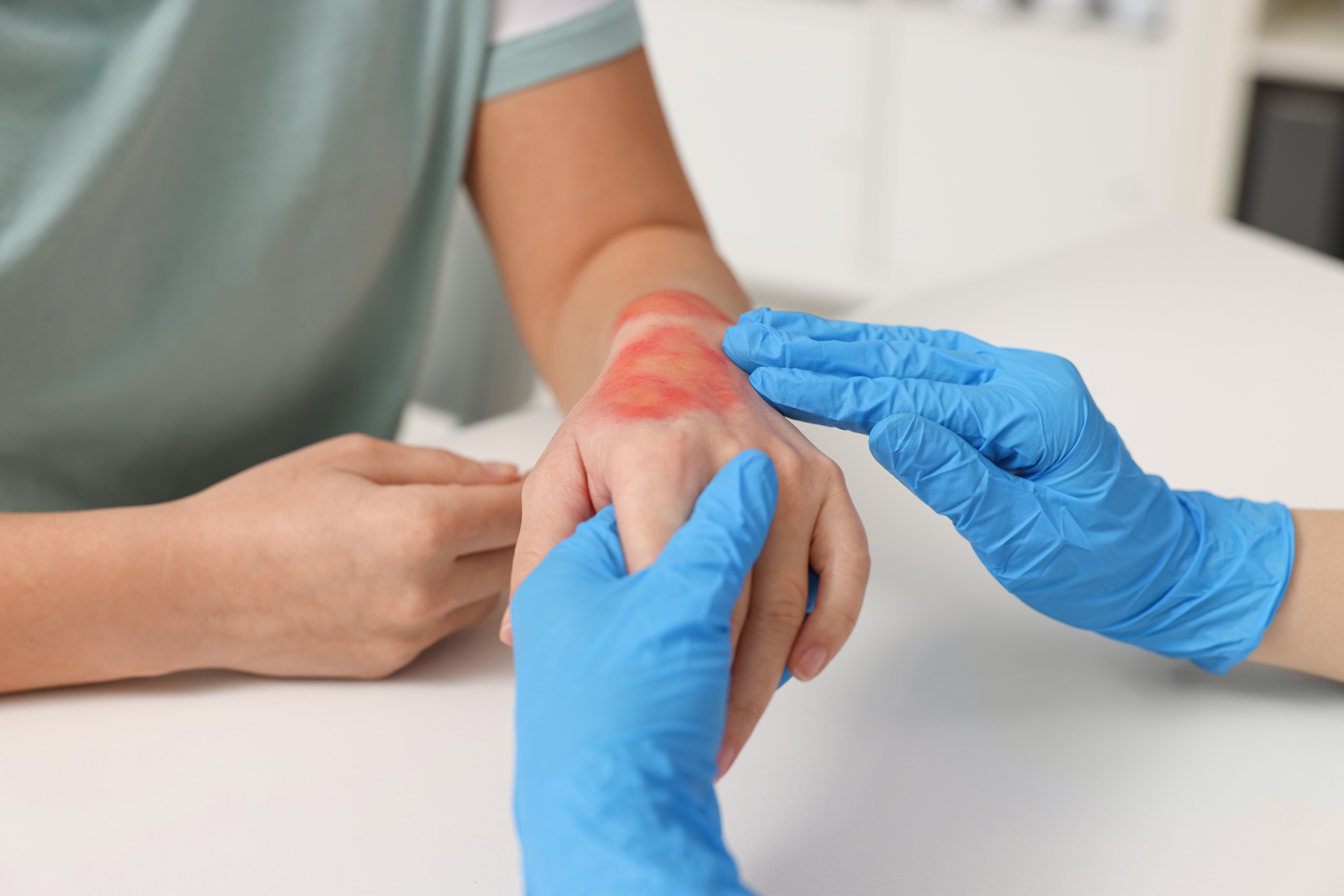
Wound care assessment plays a central role in clinical decision-making and directly influences how effectively a wound heals over time. It involves a structured evaluation of the wound’s physical characteristics, the surrounding skin, and the patient’s overall health condition. Healthcare providers rely on wound care assessment to determine the severity of injury and identify the most appropriate treatment strategy. Without accurate assessment, treatment plans may be delayed or misaligned with the patient’s actual needs. This process also helps reduce the risk of complications such as infection, tissue breakdown, or chronic non-healing wounds. Consistent evaluation allows clinicians to track healing progress and adjust interventions when necessary. In many healthcare settings, wound care assessment is considered a foundational skill that supports safe and effective patient outcomes.
Common Types of Wounds Evaluated in Clinical Settings
Wound care assessment is applied across a wide range of wound types, each requiring different clinical attention and management strategies. Acute wounds, such as surgical incisions or traumatic cuts, typically follow a predictable healing pathway when properly managed. Chronic wounds, however, present more complex challenges due to underlying health conditions that delay healing. Pressure injuries often develop in immobile patients and require careful monitoring to prevent worsening tissue damage. Diabetic foot ulcers are another common category, where circulation issues significantly affect healing capacity. Venous and arterial ulcers require vascular assessment as part of the overall evaluation process. Burn wounds and trauma-related injuries demand immediate and detailed assessment to prevent infection and tissue loss. Each wound type requires a tailored approach during wound care assessment to ensure accurate diagnosis and effective care planning.
Core Principles That Guide Wound Care Assessment
Wound care assessment is guided by several key principles that ensure consistency and accuracy in clinical practice. A patient-centered approach is essential, meaning the evaluation considers not only the wound but also the individual’s overall health status. Holistic assessment includes reviewing medical history, lifestyle factors, and existing medical conditions. Clinicians also focus on identifying risk factors that may delay healing or increase complications. Observing early warning signs of deterioration is critical in preventing further tissue damage. Standardization in assessment practices helps reduce variability between different healthcare providers. Proper communication between care teams ensures that wound care assessment findings are effectively shared and acted upon. These principles collectively support better healing outcomes and more efficient clinical management.
Step-by-Step Wound Care Assessment Process
The wound care assessment process follows a structured sequence to ensure no critical detail is missed during evaluation. It begins with gathering patient history, including past medical conditions, medications, and previous wound occurrences. Clinicians then perform a visual inspection to observe the wound’s appearance and surrounding skin condition. Accurate measurement of wound dimensions such as length, width, and depth is essential for tracking progress over time. The stage or classification of the wound is determined based on established clinical guidelines. Evaluation of surrounding tissue helps identify signs of swelling, discoloration, or infection. Documentation of findings ensures consistency and continuity of care across healthcare providers. This systematic process forms the backbone of effective wound management.
Tools and Technology Used in Wound Care Assessment
Modern wound care assessment relies on a variety of tools and technologies to improve accuracy and efficiency. Traditional measurement tools such as rulers and probes remain widely used in clinical settings. Digital imaging systems allow healthcare providers to capture detailed wound images for monitoring changes over time. Mobile applications designed for wound tracking provide real-time data collection and analysis. Pressure mapping devices are used to assess areas at risk of pressure injuries in immobile patients. Diagnostic laboratory tools may also be used to identify infections or underlying conditions affecting healing. These tools enhance precision and support evidence-based decision-making in clinical practice.
Below is a simplified view of commonly used tools:
- Sterile wound measuring rulers
- Digital photography systems
- Portable ultrasound devices
- Pressure mapping mats
- Mobile wound tracking applications
- Laboratory culture testing kits
Each tool contributes to improving the accuracy of wound care assessment and supports better clinical outcomes.
Evaluating the Wound Bed and Surrounding Tissue
A detailed evaluation of the wound bed is a critical component of wound care assessment. Clinicians examine the types of tissue present, such as healthy granulation tissue or necrotic tissue that may require removal. The amount and type of wound exudate provide important clues about the healing process and potential infection. Odor assessment can also indicate bacterial activity within the wound. The condition of wound edges helps determine whether the wound is progressing toward healing or deteriorating. Surrounding skin is evaluated for redness, warmth, or maceration, which may signal complications. These observations collectively guide treatment decisions and dressing selection. Careful analysis of the wound bed ensures a more targeted and effective care plan.
Detecting Infection and Complications Early
Early detection of infection is a vital aspect of wound care assessment because it directly affects healing outcomes. Local signs of infection include increased redness, swelling, warmth, and pain around the wound site. In some cases, pus or abnormal discharge may also be present. Systemic symptoms such as fever or fatigue can indicate a more serious infection requiring immediate intervention. Chronic wounds may develop biofilms, which make treatment more challenging and delay healing. Delayed healing patterns often signal underlying complications that need further investigation. Timely identification of these issues allows clinicians to adjust treatment strategies before conditions worsen. Effective infection monitoring is essential in preventing long-term tissue damage.
Pain Assessment and Patient Comfort Considerations
Pain evaluation is an essential part of wound care assessment and contributes significantly to patient comfort and treatment adherence. Pain levels are typically measured using standardized scoring systems that help quantify the patient’s experience. Acute wound pain often differs from chronic wound pain in intensity and duration. Managing pain during dressing changes is particularly important to reduce patient distress. Healthcare providers may use topical or systemic pain relief methods depending on severity. Psychological stress associated with chronic wounds can also influence pain perception. Addressing both physical and emotional aspects of pain improves overall patient well-being. Effective pain management supports a more positive healing environment.
Influence of Underlying Medical Conditions on Healing
Underlying health conditions significantly affect wound healing and must be considered during wound care assessment. Diabetes is one of the most common factors that impair circulation and delay tissue repair. Peripheral vascular disease reduces blood flow, limiting oxygen and nutrient delivery to the wound site. Immobility increases the risk of pressure injuries due to prolonged pressure on specific areas of the body. Nutritional deficiencies can weaken the body’s ability to regenerate tissue effectively. Immune system disorders may also reduce resistance to infection. These conditions require careful evaluation to ensure appropriate treatment planning. Addressing underlying factors is essential for improving healing outcomes.
Documentation Standards in Wound Care Assessment
Accurate documentation is a fundamental component of wound care assessment in clinical practice. Detailed records ensure continuity of care across different healthcare providers and settings. Standardized wound charting methods help maintain consistency in reporting wound characteristics. Photographic documentation provides visual evidence of healing progress over time. Proper documentation also supports legal and ethical accountability in healthcare delivery. Clear communication between team members is enhanced through structured records. Incomplete documentation can lead to misinterpretation and delayed treatment decisions. Consistent record-keeping strengthens overall patient care quality.
Interdisciplinary Collaboration in Wound Management
Effective wound care assessment often requires collaboration among multiple healthcare professionals. Nurses typically play a primary role in ongoing wound monitoring and dressing changes. Physicians provide diagnostic oversight and medical treatment planning. Nutritionists contribute by addressing dietary factors that influence healing. Physical therapists assist in improving mobility and reducing pressure-related risks. Coordinated care ensures that all aspects of wound management are addressed comprehensively. Regular communication among team members enhances treatment efficiency. This collaborative approach supports more effective patient outcomes.
Challenges Encountered in Wound Care Assessment
Wound care assessment presents several challenges that can impact clinical decision-making. Variability in wound presentation often makes standardized evaluation difficult. Patient compliance issues may affect the consistency of treatment and monitoring. Limited access to advanced diagnostic tools can restrict assessment accuracy in some healthcare settings. Misinterpretation of wound characteristics may lead to inappropriate treatment decisions. Complex chronic wounds often require long-term management strategies that are difficult to maintain. Time constraints in busy clinical environments can also affect assessment quality. Addressing these challenges requires ongoing training and resource improvement.
Evidence-Based Practices in Wound Assessment
Evidence-based practice is essential in ensuring that wound care assessment remains effective and reliable. Clinical guidelines provide standardized protocols for evaluating different wound types. Research studies continuously contribute new insights into wound healing processes. Healthcare professionals are encouraged to engage in continuous education to stay updated with best practices. Standardized assessment frameworks help reduce variability in clinical decisions. Integrating research findings into daily practice improves patient outcomes. Evidence-based approaches ensure that treatment strategies are grounded in scientific data. This strengthens the overall quality of wound management.
Patient Education and Home Care Guidance
Patient education is a key element of wound care assessment and long-term recovery. Individuals are taught how to maintain proper wound hygiene to prevent infection. Clear instructions on dressing changes help patients manage care at home effectively. Recognizing warning signs such as increased pain or swelling is essential for early intervention. Lifestyle modifications, including improved nutrition and mobility, support better healing outcomes. Caregivers also play an important role in assisting patients with wound management. Empowering patients with knowledge improves treatment adherence. Education enhances overall recovery success.
Innovations and Emerging Trends in Wound Care Assessment
Advancements in technology continue to transform wound care assessment practices. Artificial intelligence is being used to analyze wound images and predict healing progress. Smart dressings equipped with sensors can monitor moisture levels and infection markers. Telehealth services allow remote wound monitoring and consultation with specialists. Three-dimensional imaging provides more accurate wound measurements and tracking. Predictive analytics help clinicians anticipate complications before they occur. These innovations improve accuracy and efficiency in clinical practice. The future of wound assessment is increasingly driven by digital healthcare solutions.
Frequently Asked Questions
What is included in wound care assessment?
Wound care assessment includes evaluating wound size, depth, tissue type, exudate, surrounding skin, and patient health history. It also involves monitoring healing progress and identifying complications.
How often should a wound be assessed?
The frequency depends on wound severity, but most wounds are assessed during every dressing change or at least weekly in clinical settings.
What tools are used in wound care assessment?
Common tools include measuring rulers, digital imaging systems, pressure mapping devices, and diagnostic laboratory tests.
Can wound care assessment be done at home?
Basic monitoring can be done at home, but formal wound care assessment should be performed by healthcare professionals.
What signs indicate poor wound healing?
Signs include increased pain, redness, swelling, foul odor, and lack of size reduction over time.
How does diabetes affect wound care assessment?
Diabetes slows healing due to reduced circulation and increased risk of infection, requiring more frequent and detailed evaluation.
When should a specialist be involved?
A specialist should be involved when wounds are chronic, infected, non-healing, or associated with complex medical conditions.
Takeaway
Wound care assessment remains a critical foundation in effective wound management, guiding accurate diagnosis, treatment planning, and long-term healing success.